Meningitis in England: History, Risk and the Current 2026 Threat
Meningitis is not just a medical issue confined to hospitals and headlines.
It is a serious public health risk that affects working people, families and communities across England. The current outbreak in Kent serves as a stark reminder that infectious diseases have not disappeared, and that the conditions in which people live, work and socialise still play a major role in how these illnesses spread.
For Workers of England Union members, understanding the risks, recognising the symptoms and knowing when to act is important. This is about protecting not only ourselves, but also our colleagues, families and the wider community.
Understanding Meningitis
Meningitis has a long and serious history in England and across the United Kingdom. Before the development of modern vaccination programmes, it appeared in repeated epidemic waves, often with devastating consequences. Historically referred to as ‘spotted fever’ due to the characteristic rash associated with meningococcal septicaemia, the disease has consistently posed the greatest risk to children, teenagers and young adults.
Infectious diseases such as meningitis have followed clear patterns over time. Outbreaks often occur in waves, with cases increasing during winter months when people spend more time in close contact indoors. Adolescents and young adults play a key role in transmission, with carriage rates in this group reaching up to 25%. This means many individuals can carry and spread the bacteria without showing symptoms, increasing the risk to more vulnerable groups such as infants and young children.
The impact of meningitis has often been shaped by social and economic conditions. During the First World War, overcrowded military camps created ideal conditions for infection. In 1915, over 1,000 cases were recorded in the UK, with a high death rate. Similar trends were seen in the inter-war years, particularly in industrial and mining communities as overcrowding and poor living conditions increased exposure and transmission.
Medical Advances and the Current Threat
The introduction of sulphonamides and penicillin improved treatment in the mid-20th century. However, mortality rates remained significant, demonstrating that treatment alone was not sufficient to control the disease. The major shift came with the introduction of vaccination programmes from the 1990s onwards. Vaccines targeting Haemophilus influenzae type b, meningococcal group C, pneumococcal disease and later meningococcal group B significantly reduced the number of cases and transformed public health outcomes.
Despite these advances, meningitis has not been eradicated. Cases fell sharply during the COVID-19 pandemic due to reduced social mixing, but have since returned towards pre-Covid levels. Meningococcal group B now accounts for the majority of cases in the UK. The outbreak identified in Kent in March 2026, linked to university settings and social venues, demonstrates how quickly the disease can re-emerge and spread among young adults.
Recognising the Symptoms
Recognising the symptoms remains critical. Meningitis can develop rapidly and symptoms may appear in any order. These can include:
- A high fever
- Severe headache
- Vomiting and stiff neck
- Sensitivity to light
- Drowsiness or confusion
- Seizures
- Cold hands and feet
- Muscle or joint pain
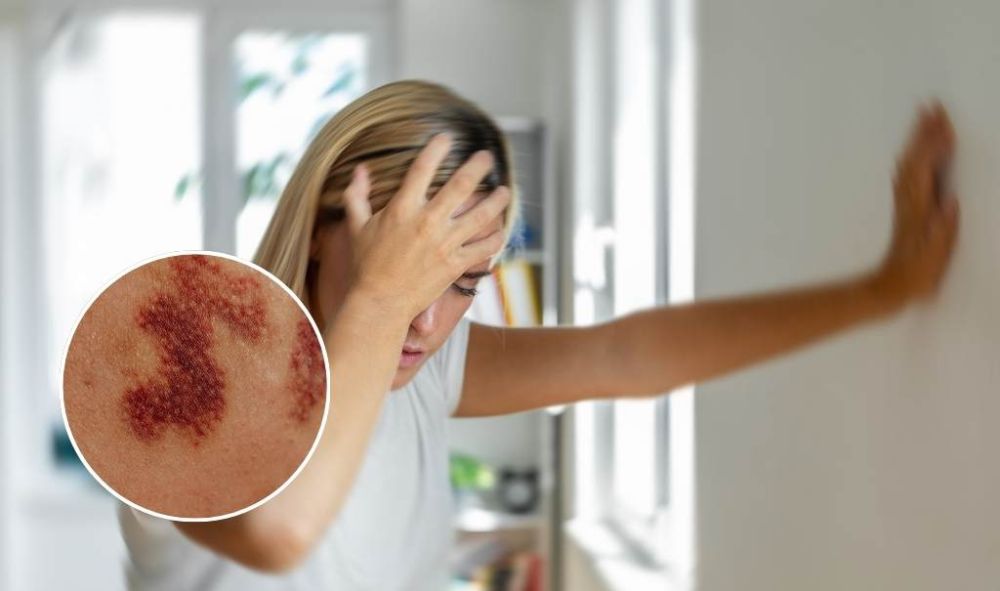
A rash that does not fade when pressed with a glass is a key warning sign, although it is not always present. Early symptoms can resemble flu or fatigue, increasing the risk of delayed treatment.
Urgent medical attention is essential. Anyone suspected of having meningitis or sepsis should seek immediate help by calling 999 or attending accident and emergency services. Early treatment with antibiotics can be lifesaving and significantly reduce the risk of long-term complications.
Stephen Morris, General Secretary of the Workers of England Union, said:
“This outbreak is a clear reminder that public health is a workplace issue as much as it is a medical one. Our members are on the frontline of communities across the country, and they need clear information, access to vaccinations and a health system that is properly resourced. No worker in England and Wales should be put at risk because of delays, shortages or lack of awareness. Early action saves lives, and we urge all members to take symptoms seriously and seek help without hesitation.”
Historical Timeline of Meningitis in England
- 1915: 1,088 cases and 434 deaths recorded, linked to overcrowded military camps.
- 1931–1932: Major epidemic particularly affecting coal-mining communities.
- 1992: Introduction of Haemophilus influenzae type b vaccine.
- 1999–2000: Peak of invasive meningococcal disease with 2,595 confirmed cases; introduction of MenC vaccine.
- 2015: Introduction of MenB vaccine for infants in the UK.
- 2020–2021: Significant decline in cases during COVID-19 restrictions.
- March 2026: Outbreak of meningococcal group B in Kent linked to university settings.
References
- UK Health Security Agency (UKHSA) (2026)
- National Health Service (NHS) (2024)
- Meningitis Research Foundation (2024)
- Meningitis Now (2024)